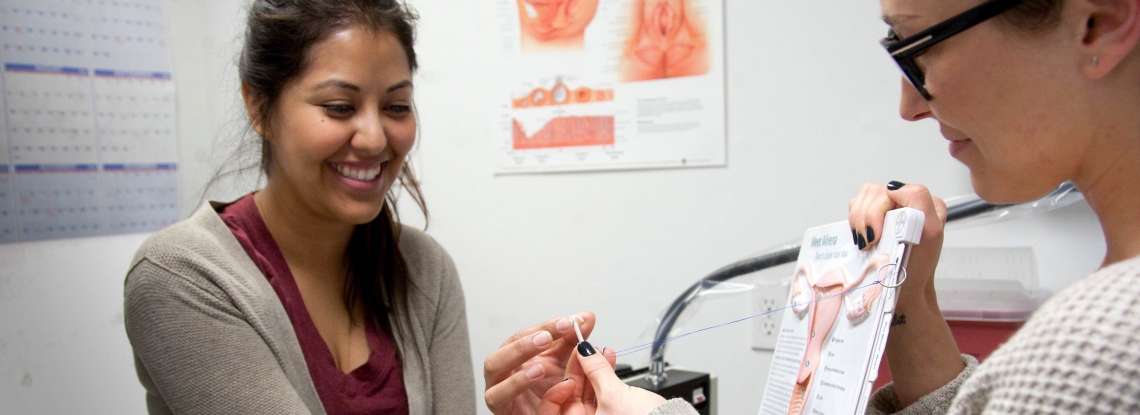
Better Birth Control Education Reduces Unintended Pregnancies
Beyond the Pill is helping to transform access to long-acting reversible contraception (LARC), IUDs and implants. Although almost all clinicians provide oral contraceptives and condoms, fewer offer IUDs or implants, which are the most effective methods of contraception. Additionally, restrictive clinic policies around patient eligibility and practices including unnecessary testing and waiting periods limit patient access to these methods. Our research, published in The Lancet medical journal, showed that an education and counseling intervention on IUDs and implants increased provider knowledge of LARC methods and evidence-based clinical guidelines for their provision. With the resulting improvements in access to these highly effective options, teens and young women at intervention sites were half as likely to experience an unintended pregnancy.
About our study
Beyond the Pill developed a training curriculum that gave health care providers the skills to educate young women about the full range of FDA-approved contraceptive methods, including IUDs and implants. The training includes information relevant to the entire clinic team (clinicians, health educators, front desk staff, clinic managers, and billing experts). Our training is designed to help providers integrate IUDs and implants into routine contraceptive care by improving method-specific knowledge as well as allowing time for practice and refinement of counseling and placement skills.

In partnership with Planned Parenthood, we rigorously tested whether the training improved access to birth control and reduced rates of unintended pregnancy in a cluster randomized trial at 40 health centers nationwide. The study followed 1,500 women ages 18 to 25 who received contraceptive counseling and did not want to become pregnant in the next year for one year, learning about their health and well-being at regular intervals. The study also evaluated the knowledge and practices of 500 clinic staff at participating clinics.
Findings
The study shows that our training program made a measurable difference in patients' lives. This randomized clinic intervention was the first to successfully help women prevent unintended pregnancies. Women receiving care at trained clinics were:

- More knowledgeable about contraceptive options.
- More likely to choose an IUD or implant.
- Half as likely to experience an unintended pregnancy over the following year (in family planning clinics settings).
For patients seeking post-abortion contraception, fewer than half who were interested in IUDs and implants actually obtained their selected method. Significant cost barriers prevent many patients from obtaining their contraceptive method of choice at the time of abortion in the US, and this finding emphasizes the need to ensure access to the full range contraceptives in all health care settings.
Our training increased providers’ knowledge about the most effective birth control options and expanded access to these methods. Providers who received the training were:
- More likely to have evidence-based views of which patients can safely use IUDs and implants.
- More likely to discuss these methods with their patients.
By increasing access to accurate and comprehensive information about birth control, our training supports reproductive autonomy and choice. More than 99% of participants in the study reported that they chose their birth control method themselves or together with their provider - regardless of whether they received care at an intervention or control clinic.
Implementation science: Taking the training intervention to scale
Our training is the first rigorously tested, cost-effective, and replicable clinic-based intervention to improve provider contraceptive knowledge, skills, and counseling to help patients access the full range of contraceptive methods. We are scaling up this intervention, and our efforts, combined with those of other organizations, will contribute to a nationwide increase in contraceptive access. To date, our trainings have reached more than 6,700 health care providers serving more than 2.4 million contraceptive clients each year.
Learn more about the national impact and value of our trainings.
Closing the gap
The development of our clinic-based training intervention to improve contraceptive education and counseling was informed by prior research. We conducted a series of studies, including in-depth interviews and national probability surveys with contraceptive providers, to better understand current practices and opportunities for enhanced service delivery.
Our research revealed large gaps between clinical practice and evidence-based guidelines for long-acting reversible contraception (LARC) including:
- Infrequent counseling on IUDs and implants, misinformation leading to overly restrictive patient eligibility, and low provision of these methods.
- Limited access to IUDs and implants due to a lack of trained providers, multiple visits requirements, and cost and billing barriers.
- The need for evidence-based training on IUDs and implants for all clinic staff, including clinicians, health educators, front desk staff, and administrators.
Our training intervention was designed to close the gap between clinical practice and the evidence on IUDs and implants. By improving contraceptive education and counseling and access to highly effective contraception, our training has helped to improve contraceptive care and access in the US.
Selected Publications
-
Harper CC, Rocca CH, Thompson KM, Morfesis J, Darney PD, Westhoff CL, Speidel JJ. Reductions in pregnancy rates in the USA with long-acting reversible contraception: a cluster randomised trial. Lancet 386: 562–568, 2015.
-
Biggs A, Harper CC, Brindis C. California Family Planning Health Care Providers' Challenges to Same Day Long-Acting Reversible Contraception Provision. Obstetrics & Gynecology 26(2): 338–345, 2015.
-
Harper CC, Stratton L, Raine TR, Thompson K, Henderson JT, Blum M, Postlethwaite D, Speidel JJ. Counseling and provision of long-acting reversible contraception in the US: National survey of nurse practitioners. Preventive Medicine 57:883-8, 2013.
-
Thompson KMJ, Stern L, Gelt M, Speidel JJ, Harper CC. Counseling for IUDs & implants: Are health educators & clinicians on the same page? Perspectives on Sexual and Reproductive Health 45:191-195, 2013.
-
Harper CC, Blum M, Thiel de Bocanegra H, Darney PD, Speidel JJ, Policar M, Drey E. Challenges in translating evidence to practice: the provision of intrauterine contraception. Obstetrics & Gynecology 111:1359-1369, 2008.